Dental Implants
Dental implants – replacement for missing teeth
Dental implants represent the best treatment option for missing teeth. The dentist implants an artificial tooth root in place of the missing tooth. After a few weeks of healing and growing time, this implant becomes very solidly fixed into the jaw bone. This dental implant can then be used as a robust foundation to fit a crown, bridge or a prosthesis (denture). A new tooth is created: strong, durable, and feeling like a normal tooth. The implants are completely compatible with the human body, and create a great impression visually. This is the true value of implantology: teeth can quite literally be replaced.
One of our experts would be delighted to advise you further in a non-binding consultation appointment about our implants, available either in Konstanz or Bietingen near Schaffhausen. Implants fall under a highly-specialised field of dental medicine, and so meaningful treatment recommendations can only be made after careful diagnostic tests are carried out on a case-by-case basis.
We can clarify all your questions during these consultations:
- Dental implants made from titanium or ceramic materials?
- Do I have sufficient/too little jaw bone remaining, and do I need a bone grafting procedure?
- Are the surrounding teeth solid and free from periodontal disease?
- How compatible are the implants with the body?
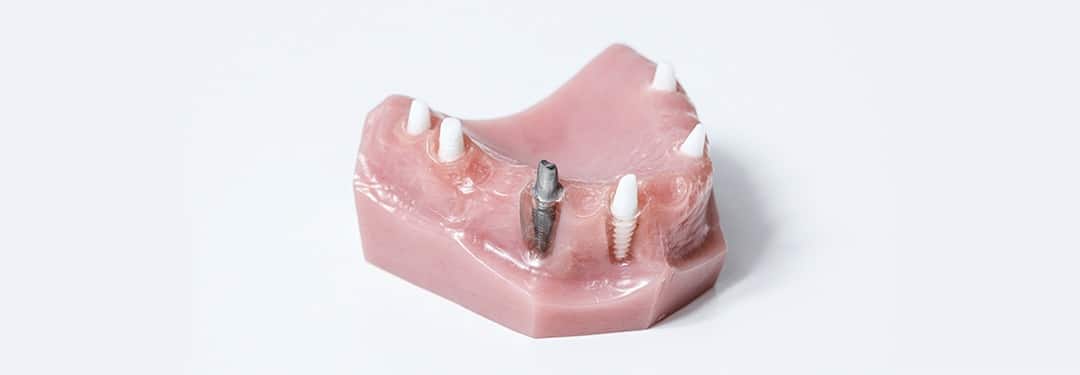
Dental implant consultations
We have a specialist team available for consultations on dental implants, bone grafting and for any other questions at both the Dr. Hager Dental practices, in Konstanz and in Bietingen near Schaffhausen. Cutting-edge medical equipment and machinery, such as digital volume tomography devices (“DVT”, “CB CT”) support our work with reliability and precision during our planning of implant treatments. This complements our firm basis of the years of experience of our implantologists, Dr. Michael Hager, Benjamin Hager and Dominik Hager, with many hundreds of implants provided each year. All of this contributes to our dental teams in Konstanz and Bietingen achieving the best possible result for you.
Make the most of a free appointment with us in which we will provide you more information and answer any questions you might have on dental implants and bone grafting: all of our expertise in a one-to-one, personalised appointment with you.
You can obtain personalised information about dental implants in Konstanz or Bietingen, either over the phone or using our online form page.
Implantation with CT-based navigation
After a comprehensive consultation and subsequent treatment planning, the implant is inserted.
It then fuses slowly as the jaw bone grows around it. You can find out exactly how this process occurs on this page.

1. Initial examination and consultation
Before an implant procedure can be performed, an extensive consultation is carried out during which all the patient’s wishes, treatment options and any risks involved are discussed. We carry out precision imaging of the jaw bone and mouth region, and take a history of your lifestyle factors and general condition of your health.
The planning phase then follows. Our many years of experience combined with cutting-edge diagnostic approaches ensure that we can provide the best possible planning for the desired procedure. Digital X-ray imaging and, where needed, computer tomography techniques create extremely precise renderings of the jaw structures and form the fundamental basis for planning.
2. The implantation procedure
When the day of the implantation procedure comes around, the following steps are followed: After local anaesthesia is applied, an incision is made in the gums. A special drill is then used to create a high-precision hole in the jaw bone.
Finally, the root-shaped implant is inserted into place and the gum is closed back up with stitches. After a healing time of around 2 months, bone and implant become solidly fused together.

3. The healing phase
For the implant to heal quickly and naturally, fusing with the bone, the treatment area must be carefully protected for a certain period after the procedure. The duration of the healing phase depends on factors such as bone quality and the quantity of available bone. On request, a provisional denture can be created for use after the implantation procedure in order to preserve the appearance of the teeth (common where the incisors are affected).
You should take particular care to avoid anything that might put stress of the treatment area in the first few days following the procedure. This also means plenty of attention and care when cleaning the teeth and gums, and avoiding solid food.

4. The prosthesis (denture) is fixed into place
Once the implant has healed into place and has fused solidly with the bone, we manufacture crowns in our dental laboratory. These are then securely fixed onto the implants.
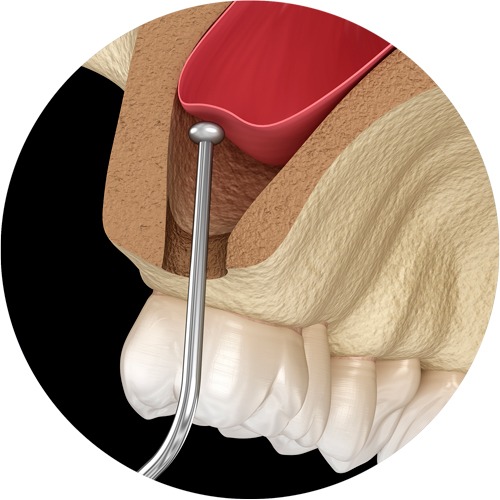
5. In cases where there is insufficient bone
Where not enough bone exists for an implant to be inserted, a bone graft procedure can be performed. A variety of different surgical techniques are employed in order to fix an artificial bone material onto the existing jaw bone in order to create a reinforced basis for the future implant.
These techniques include: sinus lifting, bone augmentation procedures, splitting, spreading, and more. A longer healing time is required in the case of these procedures.

6. How long dies the treatment process last?
How long the whole treatment process takes, including healing time, depends significantly on your medical condition, and may vary from two weeks to six months.
A very quick treatment option, involving a process referred to as “immediate loading” is an exception, but may only be carried out when conditions are very good. In general, the entire duration of treatment is around 3 months.

„The treatment process for implants depends on many factors. Bone quality and the quantity of bone available are fundamental aspects to successful implantation. Our high standard is reflected in the use of our 3D X-ray imaging devices in the case of our implant procedures. Using this 3D imaging technology, the DR. HAGER | Dentists can perform a fully-navigated implantation. This offers our patients the highest levels of safety and ensures we maintain our high success rates and meet our strictest requirements for our patients’ well-being.”
Dominik Hager, Dentist at the Dr. Hager Dental Practice
Properly care for new teeth after dental implantation
When properly cared for, and with regular check-ups, implants are very likely to last an entire lifetime. Implants represent a great investment, offering a range of benefits. You should take care of your implants in exactly the same way as you would go about caring for natural teeth. In this way, you will be able to continue to enjoy the benefits of your new teeth over a long period of time.
Plaque deposits contain bacteria, and this bacteria can cause inflammation. This type of inflammation puts both teeth and implants at risk.
As such, it is vital to look after the teeth (natural or otherwise) using suitable cleaning tools and techniques. We are always happy to advise our patients further.
In addition to good oral care at home, we recommend regular check-ups and maintenance appointments with the professional dental hygienists working in our practices. This ensures that stubborn deposits can be removed, as well as providing general care, and special treatments can be applied to ensure your implants are kept in flawless condition.
Case studies with dental implants
When we are born, we might not be able to show off our teeth to anyone, but they are already present in our mouth even as babies. Over the course of your life, teeth are put under lots of stresses and strains, and this takes its toll. People who end up losing their teeth want to find a good replacement solution. These replacements should look as natural as possible, and function flawlessly. Dental implants can be used in all patients after age when the bones have stopped growing. Even advanced age is rarely a reason for implants not to be used. An ideal solution can be found for almost every single case.
Tooth loss can affect people of all ages:
due to sports and games; through tooth decay; or inflammation of the periodontium (periodontal disease/periodontitis). Poor dental hygiene and/or a poor diet can also damage the teeth.
Modern X-ray technologies support the procedures we carry out.

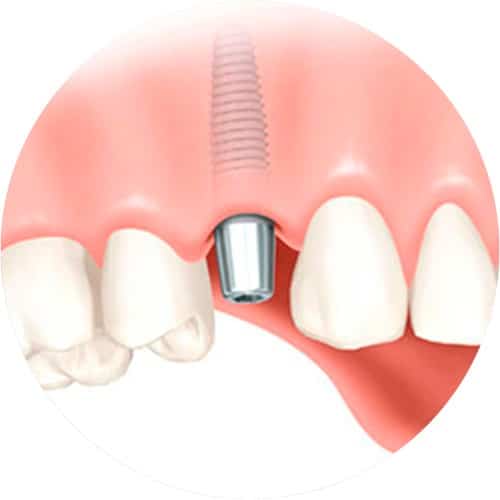
Missing a single tooth
If a single tooth is lost, the resulting gap can be closed using an implant. With this treatment, the adjacent teeth are not used to support the replacement tooth, and so do not need to be prepared (involving grinding down of the natural teeth). In terms of how the results look, too, implant treatments are often the best solution when compared with conventional treatments. Modern ceramic materials are particularly able to perfectly reproduce natural teeth.
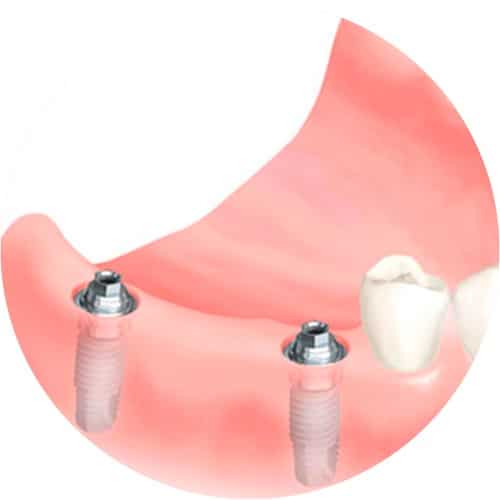
Several teeth missing
In cases where several teeth have been lost, the resulting gaps can be closed using implants. In this treatment, the implants act as supporting pillars for replacement teeth. Cases of several back teeth missing at the end of a row of teeth represent a special situation. In these cases, implants are the best and only solution available to carry a replacement tooth (with the exception of a removable prosthesis, with their many disadvantages). Using implants makes it possible to avoid mechanical retaining elements (e.g. brace wires) that negatively affect both the appearance and comfort of the final treatment.
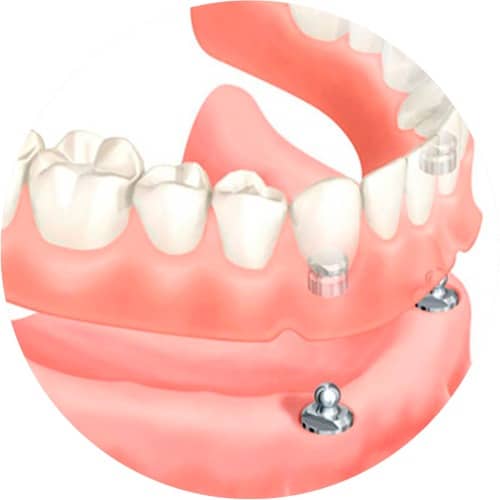
All teeth are missing
Even when all teeth are missing, there is a far better solution available than the conventional ‘full prosthesis’, as even in these cases, there are implant treatment options that can be used. Depending on the exact requirements, needs and patient objectives, either a fixed or removable prosthesis solution based on implants can be created. Many removable prosthesis wearers complain about poor comfort levels when using their prosthesis and painful pressure points. Adhesive creams and mechanical solutions can solve these problems, but are often not permanent and produce unsatisfactory results. Thanks to their solid anchoring in the jaw, implants used in combination with a prosthesis can be the perfect solution for these cases. The most comfortable solution is a complete implant-supported prosthesis.
Dental implants – the surgical procedure in detail
Many different paths can lead to the same goal: the same also applies in dental medicine. With the many different surgical and treatment options available that use implants, a great many different approaches have been developed to date.
This makes it more and more difficult for patients to get an overview of the options available to them. The following article is intended to give you an overview of the standard procedures available in modern implantology.

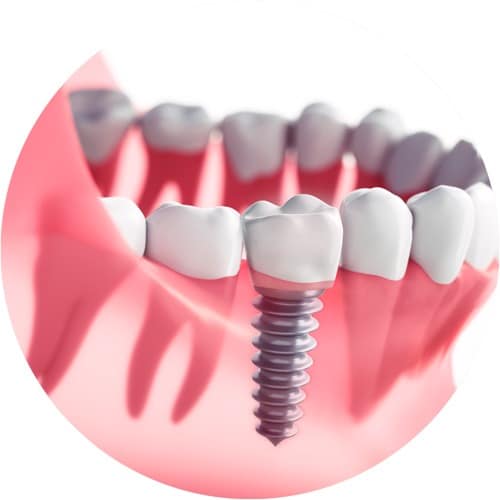
Implantology with or without bone grafting
Conventional safety-based implantology is a traditional method that was developed in the 1960s for titanium implants. A hole is drilled into a section of healthy bone with the same shape as the implant for insertion. The implant is then inserted using a little pressure, or screwed into place. If any artificial bone grafting is required, this can be performed during the same surgical procedure. Due to the roughened outer surface of the titanium implant, the bone grows and fuses within around two months.
After this time, a permanent and extremely robust connection is formed between bone and implant. Only once the bone and implant are solidly fused together is the planned tooth replacement then affixed to the implant itself. Subsequent to this, chewing and stressing of the implant can occur.
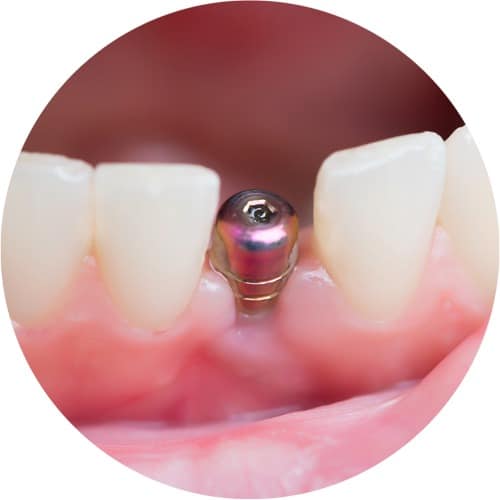
Immediate restorations
In immediate restorations, an implant is set directly into the fresh wound left behind on removal of a natural tooth. This procedure generally requires for the underlying bone structure to be free of inflammation and be sufficiently stable in order for the implant to immediately find a secure hold in the jaw.
Where only a small area needs building up, bone grafting can also be carried out during the same procedure. This procedure is particularly employed in the incisor area as it ensures the best option for preserving the appearance of the gums. These advantages, however, come with the disadvantage of increased infection risk.

Immediate loading
Immediate loading is the term used when the desired prosthesis is immediately affixed to the implants that are set as part of immediate restorations. This has the advantage that the desired appearance (a complete row of teeth) can be achieved immediately after removal of the diseased teeth. This advantage is once again, however, bound with an increased risk of implant loss. Even in the case of the fastest treatment methods, the bone must be left to heal over a period of eight weeks, fusing with the implants.
Implants immediately supplied with crowns, therefore, pose a particular challenge in terms of how patients understand the treatment and any given patient’s self-discipline, as the new teeth must be very carefully protected for this time. Unfortunately, these requirements are not mentioned enough in the press or in advertising. It is very rare for an implant provided using this procedure to fuse correctly without the proper protection and care.
Implantation with CT-based navigation
Since 1996, we have been using this highly sophisticated implantation technique. During planning for the procedure, computer tomographic imaging is carried out (“ConeBeam CT”, “DVT”) on the jaw using a prepared template created by us in practice. This allows our dentists to carry out comprehensive planning: the type, size, and best location of the implant(s) to be inserted can be planned ahead of time with computer-based three-dimensional rendering.
During the surgical appointment, implants are set into the exact positions as planned, using the templates as a guide. As a result, a previously manufactured provisional, or even permanent prosthesis can be affixed to the implants straight away, a type of immediate loading solution (see above). This clearly represents the fastest treatment option available and this is the reason why it has also drawn significant media attention.
However, by summing up the different inaccuracies that are involved in the process, it becomes clear that the standard precautionary and safety measures applied generally in implantology are also necessary in cases where these newer technologies are applied.
Even the savings in terms of time are only possible if no bone grafting procedure is required, as in this case, a surgical procedure must be carried out approx. 6 months beforehand, and the graft be fully healed before implants can be inserted.
In this case, then a second surgical procedure is required after the bone grafting surgery in order to insert the implants, compared to the conventional safety-based practices with just a single surgical procedure (implantation with simultaneous bone grafting).
For this reason, we only apply this treatment approach where the surgery can be carried out in a single appointment i.e. where no bone grafting is needed. This is because it is only in this case that this method can offer additional advantages to the patient.
Implantation systems
The vast world of implant systems can seem very diverse to patients investigating their treatment options. In order to give you a little insight into the different systems available, and thus explain their underlying philosophies, we want to first provide some essential facts: The aim of a dental implant is to come as close as possible to the model example set by the natural tooth.
Implants consist of a root part, which is anchored into the bone, securely attached to the crown section, which extends from the root just like natural tooth’s crown, fulfilling the diverse functions of the tooth. Also vitally important are the chewing and speaking functionalities and appearance of the implant.
The beginnings of implantology development took place in Scandinavia (I. Branemark 1960), then spreading to the USA, Germany, Switzerland and then expanding worldwide. The ‘silicon valley’ of implantation development has been right here in our midst for many years now: the region around Lake Constance – Black Forest – Jura is home to the majority of developers and researchers of the implant industry. Well-known manufacturers such as Straumann, Nobel Biocare, IMZ, Camlog, BioHorizons, Frialit, Ankylos, Bauer and SDS Volz have based their research and development locations here.
Swiss, German and a few US companies dominate the market. Dental implants may be considered somewhat similar to the watch-making industry due to their intricacies and detailed precision, innovation, and the committed workforce dedicated to both fields. At the same time, developers must have a high level of knowledge and expertise similar to that required when working with medical technologies.
In our region, these branches have known development clusters: Tuttlingen, Basel, Pforzheim, Mannheim, Belfort, Heidelberg.
The materials using in dental implants have not fundamentally changed since they first appeared on the market: titanium came first, and ceramics soon followed. The shape of implants changed from quite bizarre shapes, such as grids, needles, plates, and tubes up the implants that prevail today, generally with screw-shaped roots. The structural upper part for the dental crowns has also varied, from pre-fixed designs, to screw-in designs or cemented conical shapes. All the possible technical solutions imaginable are still constantly being tested in the search for the very best solution.
Here is a brief overview of the main producers working in implantology and the main features of their products:
Straumann 2 product lines, screw-based design, rough titanium surface, screw-in design for affixing the cro
Nobel Biocare 7 product lines, technically similar with rough titanium surfaces and screw-in abutments
IMZ Early implantation system with elastic abutments and extremely rough titanium surfaces
Camlog 3 3 product lines, all similar in their titanium surface design, but with both push-in and screw-in designs
Ankylos 2 product lines, rough titanium surfaces with deep threads, conical push-in designs and screw-in designs
Bauer Prototype for one-piece implant with a deep-tapping screw thread and rough titanium alloy surface
SDS Volz 4 Experimental product lines, early ceramic implants of the new 4th generation, with screw-in ceramic design
For both titanium and ceramic implants, new products are constantly being developed and launched to market with a wide range of different features. As is often the case with medical products, the accompanying critical scientific evaluation and rigorous testing cannot keep pace with the constant influx of new product features. As since the basic characteristics of the products have only been tweaked by manufacturers, however, your dentist will be able to rely on a high reliability of the implants.
Here are a few more interesting aspects which are considered by your dentist when selecting the right implant system for each individual case:

1. Bone quality
Different bone qualities require a suitable type of screw thread and a different basic shape for the implant body. As such, in the case of soft bones, “D4” (often the case in the side areas of the upper jaw) a rough, more protruding thread is better for the primary fixing, i.e. the implant fixing into place directly after first screwing in. In this way, very loose bone tissue can initially be fixed; a conical implant will hold more firmly in place in comparison with a parallel-walled one. On the other hand, this dental implant would require a great deal of effort to fit during primary fixing in the case of very hard bone, “D1” (e.g. in the side areas of the lower jaw).
In these cases of extremely hard bone, a thread must be cut out into the bone before an attempt can even be made to screw the implant into the bone. All of these aspects are not relevant, however, when it comes to the secondary fixing (the fixing of the implant into the jaw that is achieved after it fuses with the bone), which is the aspect which is actually more important. In this respect, the important features are the microscopic surface structures found on the titanium or ceramic material.
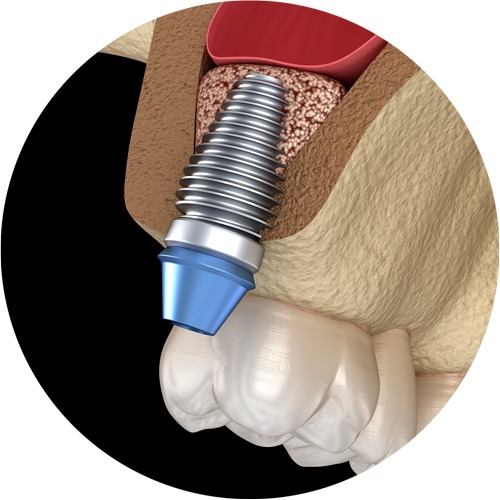
2. Suitable thread for the implant concept
This category also covers implantology considerations regarding which threads are best suited for use in immediate-loading or subsequent-loading treatment approaches. Currently there is a boom in the use of wide-threaded screw types: it is believed that the high-quality primary fixing leads to undisturbed fusing of the bone during the later healing phase. As such, they are better suited to immediate-loading treatment approaches used by dentists.
On the other hand, dentists have to take a significantly greater pressure exerted on the cells that are growing during the sensitive bone growth phase into consideration when using this treatment approach. Many implantologists do indeed try to actively and quickly reduce this pressure exerted by the dental implant after it is screwed into place.
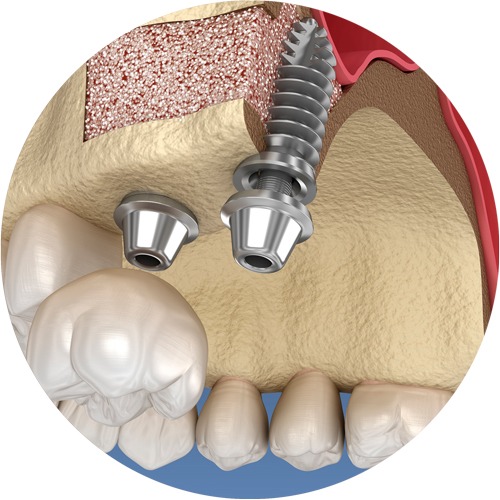
3. The anchorage of the so-called crown abutment or attachment
Another interesting aspect that must be considered is how the crown body or ‘attachment’ is anchored onto the implant body. Here we can find the traditional screw-on abutments that give a certain degree of protection against rotation and tilting. Unfortunately, the easy-to-use “external hex” screws have frequently suffered from screws becoming loose, or even fractures occurring.
This is really disastrous in cases where a larger bridge is fixed onto an implant of this type. Due to the loosening of just one screw, the entire reconstruction would generally have to be replaced. This is the reason why all manufacturers have at least one product line with a friction-locking connection formed on the interior part of the implant, in either conical or parallel tube designs. For these solutions, fitting tends to become much more complicated for the dentists: even on inserting the implant, great care must be taken to ensure an identical screwing direction for implant and abutment. This is not easy, as often the structure of the bone itself determines the screwing direction for the implant. As a consequence of this, there was pressure on the developers and manufacturers to develop a more adaptable system. Using special new surgical and prosthetic protocols (P. Malo, 1990), an extreme angle deviation of more than 30 degrees was required, with corresponding updated drilling techniques. This technology has been made possible through the use of multiple screwed abutments in dental medicine.
Over the course of these developments, it also became clear, for example, that the earlier requirements were not necessary with implants inserted in as parallel a way as possible. The requirement for bridges based on teeth and implants to be able to compensate for mobility turned out to be just as dispensable. The concerns regarding a need to interlock teeth (movable) and implants (immobile) were proven to be unfounded in the 1980s. Rather, just a few important techniques had to be employed during treatments, including special preparation of teeth.
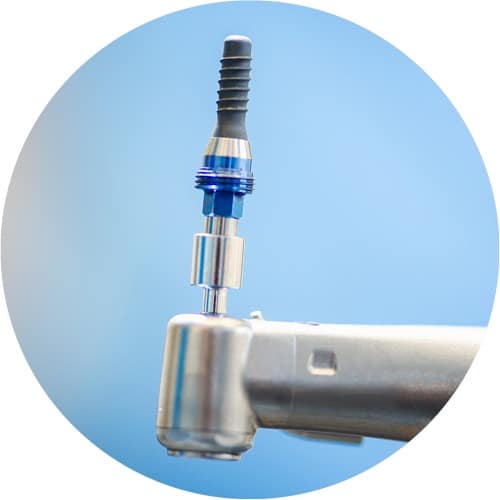
4. The right drilling technique
Drilling techniques have also changed radically over the decades: initially it was believed that higher drilling speeds and correspondingly intensified cooling would create the most exact possible hole for implantation.
After a few years, dentists started to become more convinced of that fact that holes drilled at lower speeds, with slightly smaller dimensions and therefore using less cooling and still ensuring no damage due to heat production ensured the best healing of implants.

5. Cementing or screwing in the implant
Currently, there is extensive debate on whether it is more beneficial to cement or to screw dentures onto the implant. Both techniques can even be combined, making the debate even more interesting. If crowns are cemented onto implants, there is always the risk that the cement can end up reaching under the surrounding gums and onto the rough implant surface. This then triggers an inflammatory response in the surrounding bone which can put the long-term stability of the implant fixed into the bone at risk. Cementing the crowns does, however, make it easier to fine tune the positioning and height of several implants connected through bridges. Poor positioning leading to incorrect distribution of forces through the implants would also lead to inflammation in the bone and around the implants (‘periimplantitis’). Using cement also ensures that micro-fissures formed between abutments and the screwed-on crowns are sealed tightly against bacteria. This ensures that any accumulation of particularly dangerous anaerobic bacteria (periimplantitis) can be prevented. By screwing on special intermediate pieces milled out using CAD-CAM processes (using bonding adhesives) an attempt is made to combine both advantages whilst overcoming the disadvantages. Special techniques are applied in the dental laboratory in order to achieve this.

Conclusion implant systems
It is always amazing to observe how very compelling fundamental treatment principles can be proven to be either superfluous or even turn out to be false over time. A lot has been learned, and is still left to be discovered by both the scientific communities, dentists and industry. The mechanics of living tissue, and its ability to adapt to changing conditions never ceases to astound researchers as they investigate further.
At the same time, it is becoming increasingly clear how important the biological regeneration of bone and gum tissue is for the multi-stage healing process of implants in the bone. It is becoming clearer that a variety of medicines, lifestyles, toxins and habits all have an influence on the healing process.
To improve planning in implantology, we first created a three-dimensional X-ray image with the computer tomographs used in radiology before operating on a dental implant. This allowed us to determine the spatially correct position of the dental implant already in the planning phase. In the 2000s, a new X-ray technology was developed: digital volume tomography (DVT).
Our dentists could now elegantly measure the three-dimensional representation of the bone and even the mucosal structure with high visualisation accuracy. Thus was born guided surgery, also known as three-dimensional controlled implantation. In order to expand this visualisation possibility with a drilling aid created using this data prior to the implantation, a guiding technique with drilling templates or even drilling robots was developed: navigated implantology.
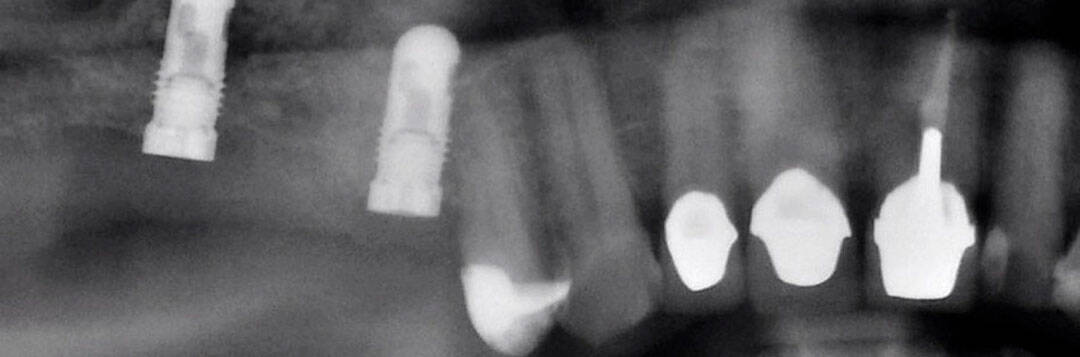
Since 1996, we have been using this particularly advanced form of implantation technology, initially on the basis of computed tomography. To plan the procedure, our dentists take a computer tomographic X-ray image („ConeBeam-CT“, „DVT“, Digital Volume Tomography) of the jaw with a template prepared for your jaw in our practice, with the cooperation of our laboratory. A special X-ray machine that uses digital volume tomography is available in both practices of DR. HAGER | Dentists in Schaffhausen and Konstanz is available. It is used to prepare for and also during implantation. This now allows our dentists to carry out comprehensive planning: the type, size and best location of the future dental implants are planned in advance in three dimensions with the help of a computer. The planning programmes used for this („SimPlant“, „Sicat“, „Impla“, „Orange“, …) process the data from the digital volume tomogram DVT created for the planning and bring them into connection with the data of the jaw (matching). They show the dentist the size and three-dimensional shape of the bone.
With true-to-scale digital representations of the desired implant types and sizes, it is possible to generate a good simulation of the expected three-dimensional position of the implants in the existing bone. This position is then transferred to a drilling template via a digital or analogue technique.
During the surgical session, guided by this drilling template or a digital drilling robot, it is possible to place the implants exactly in the intended location. Like a ship guided in the right direction by a lighthouse signal, the drill and then also the implant are navigated to the right place by the drilling aid: navigated implantation. Because of the planned position of the implants, a provisional or even final prosthesis made by the dental technician can be inserted by the dentist immediately after the procedure. This is clearly the fastest type of restoration in implantology, and the enthusiasm in the media is correspondingly high.
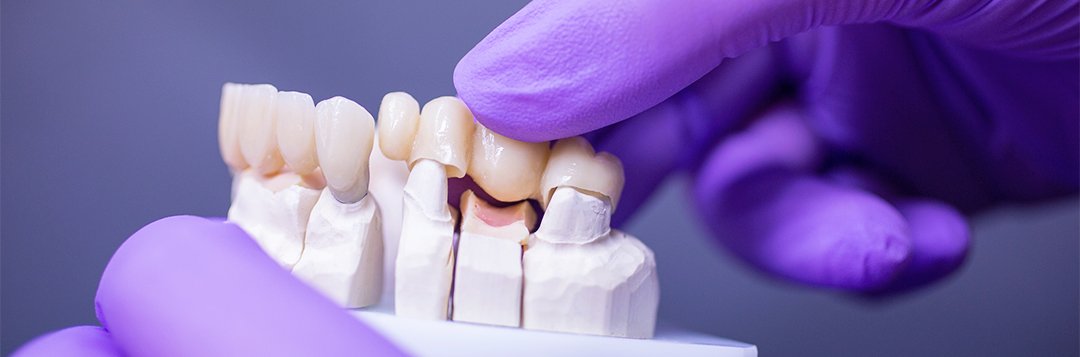
However, the high number of work steps in planning and the complex measurement and control algorithms means the sum of inaccuracies increases. By summing up the various procedure-related inaccuracies (up to approx. 2mm and 30 degree angular deviation), the usual precautionary measures and safety distances in implantology are then also necessary in navigated implantation. However, with the proximity of nerves, maxillary sinus and neighbouring teeth, the distance from the implant must be precisely maintained.
With the scaled measurement methods we use during surgery, a higher accuracy can now be achieved than with navigated implantation. Therefore, the use of computer-navigated implantology no longer seems indicated to us in many situations, as it is more likely to be sufficiently safe when there is already a sufficient supply of existing bone. However, in such a situation, navigation is not really necessary at all.
Restoration with dental implants with navigated implantation
Moreover, the emphasised speed of restoration with dental implants using navigated implantation is achievable only if bone augmentation does not have to be operated on at the same time. Compared to the conventional safety procedure with a single operation (implantation with simultaneous bone augmentation), with navigated implantation a second operation is necessary to insert the implants after the operation for bone augmentation.
Therefore, we use conventional navigated implantology only if the operation can be completed in one session, i.e. if no bone augmentation is required. Only then does this method result in a time advantage for the patient.
Procedures in navigated implantology
A particular advantage of computer-navigated implantation is that it avoids opening the mucosa. An operation is not necessary because the bone no longer has to be visible for the drilling. We do a large part of our implantations without opening the mucosa. The accuracy of the three-dimensional assessment of the bone shape can be reliably achieved by digital volume tomography DVT and the conventional clinical examination. Navigation by a drilling template or a drilling robot is rather disadvantageous for the precision compared to the guided surgery by scaled intraoperative measurement (SIM), which we prefer. This technique achieves maximum protection of the jaw without opening the mucosa through minimally invasive surgical technique while at the same time achieving the highest precision and safety through the methods of guided surgery.
Videos of the denture treatments – DR. HAGER | Zahnärzte
Here you will find short and informative videos about some of the treatments we offer in our practices DR. HAGER | Dentists in Bietingen and Constance near the Swiss border.
Videos on treatments with implants
Videos of treatments with inlays and crowns
Total Denture Videos
Dental implants – Frequently asked questions
In our FAQ of DR. HAGER | Dentists we have summarised the most frequently asked questions about dental implantation and the topic of implantation. If you have any further questions, please do not hesitate to contact us, we will be happy to help you!

I have heard that implants only last for 5 years. Is that true?
No. Long-term studies show that the success rate of implants after 10 years is over 90%, on average. An expertly performed implantation procedure and careful planning of the surgery are required to achieve this. Implants can last a lifetime for patients that are in good health who attend regular dental hygienist appointments and check-ups with the dentist, and also carry out meticulous cleaning of their teeth at home.
Can implants cause harm?
This is where high levels of care and precision and specialised training are essential. It is particularly important for procedures to be thoroughly planned, e.g. using 3D tomography imaging techniques. A surgical room equipped with cutting-edge technology and devices e.g. digital real-time X-ray imaging for use during the surgery itself, increase the precision that can be achieved during surgery, and ensure higher levels of safety.
Does implantation involve any pain?
Implantation is carried out under local anaesthesia so that patients feel absolutely no pain during surgery. Only after the surgery do patients experience some generally minor complaints, which tend to clear up in the first few days following the procedure.
Do implant-supported teeth feel different compared to natural teeth?
Implant-supported teeth will give you a completely natural feeling in the mouth while speaking, eating and laughing. You will feel little difference, if any.
Are implant sometimes rejected?
Rejections as such cannot occur. However, in cases where implants are not properly cared for, inflammation may occur around the implant, which in the worst cases results in the implant requiring extraction.
How long do I have to wait after the implant surgery before returning to work?
After inserting the dental implants there may be some slight swelling and minor pain. However, most patients are able to go back to work the next day.
How long does the surgery last?
The implantation lasts between 30 minutes and 2½ hours, depending on the circumference.
When will I be able to chew normally again?
As a rule, implants can be used for chewing after 2-3 months. It is strictly the related bone-grafting procedure that has a healing time of around 6 months.
Will I be left without teeth during the treatment and during the healing periods?
If you have previously had a removable denture, in most cases you can continue to wear it after small modifications have been made. Otherwise, tooth gaps will be closed with a temporary denture. Under the right conditions, the implant can be inserted immediately, called a “long-term temporary restoration”.
How long do dental implants last?
Long-term studies show that the success rate of implants after 10 years is on average over 90%. The prerequisite for this is professional execution and careful planning of the surgery. With good health, regular dental hygiene, check-ups and conscientious home care, implants today can last a lifetime.
How much do implants cost?
Each patient requires an implant treatment adapted to their specific situation. During our one-to-one consultation with you, we will discuss costs together with you and you will go away with a cost plan, including a fixed ceiling price which we guarantee cannot be exceeded. This makes sure all the costs are clear and form a better basis for the all-important decision-making process. Good decisions require time. However, if you just want to get a price estimate, please contact our service team via our contact form.
How long does it take for the dental implant to heal?
Implants usually need 2-3 months to heal before they can be chewed on again. If bone augmentation is necessary beforehand, healing takes about 6 months. However, you do not have to spend this time without teeth: if you previously had a removable denture, you can usually continue to wear it after a small adjustment. Otherwise, the gap is closed with a temporary denture. Under certain conditions, this can be attached to the implants immediately – as a so-called long-term temporary denture.
Up to what age can implants be used?
In principle, dental implants can be used in patients of almost any age. Exceptions include children and young people whose bones are still in the growth phase. In these cases, jaw implants would affect the jaw’s growth and lead to unsatisfactory results.
How should I properly care for a dental implant?
Treat your new teeth as if they were your old ones. Implants should be cleaned regularly with a toothbrush and good oral hygiene should be maintained in general.
I‘ve heard of things like “new teeth in one hour”, “fast and fixed”, and “beautiful teeth, now” in the media. Will I really be able to chew with my new implant-support teeth straight away?
The procedures outlined above, and some other techniques, generally allow for a temporary tooth replacement solution to be fixed onto the implants immediately. This is only possible when there is a good amount of quality bone available, i.e. if bone grafting is not required. Despite this, great care is still absolutely fundamental when using the temporary dentures for the eight-week period. After this healing time, the manufacture of the final, definitive denture is begun, which is then fitted after a further two-week waiting period.
What advantages are there to the entire treatment all being carried out by one treatment team?
As you will surely have noticed, particularly within the complex field of implantology (as is also the case for all medical treatments) there are many different factors to be taken into account in any individual case. A combined approach must be developed involving both surgical considerations and the manufacture of the implant-supported dentures. Solid technical manufacturing and long-term follow-up and maintenance care must also be ensured. The extensive, initial consultation with our expert dentists is of particular importance. During this consultation, all of the treatment options mentioned here will be discussed with you with a view to extensive treatment planning. We will make all possible treatment options available to you. Every single treatment step is carried out in our dental practices and by our dedicated team of dental staff.
Why are all implants not carried out using this fast method?
It is important to note that often the faster tooth-replacement treatment with implant-supported dentures has a few advantages when compared with traditional approaches: sterile; bacteria-free conditions maintained; predictable aesthetic result; and better anchoring due to the possibility of new bone formation. In the case of teeth that have been destroyed due to severe bacterial infections, however, implantation into the infected wound is risky.
I would like to have ceramic implants. Is that always possible?
According to patient wishes, we can use either titanium or ceramic implants in each case. Our certifications and many years of experience serve as testament to the safety of the different systems available. It should be noted, however, that currently almost all available ceramic implants are “one-piece” i.e. after being inserted, they protrude around 5 mm from the gum into the mouth, but must under no circumstances be put under any stresses or strains. This means that there are far stricter demands put on patients in terms of their care and attention regarding the implants for the duration of the healing period. This is especially true if bone grafting was required. In the near future, everything will be much improved! We are currently developing our own two-piece ceramic implant, which can be left protected under the soft-tissues (gums) to heal. Only once the healing process is completed is the implant then exposed to the stresses of the mouth, as is the case with titanium implants. For the new two-piece ceramic implants that have been presented only very recently, the critical point is the connection between the “two pieces”, abutment and implant. There is still not very much clinical experience available to refer to concerning long-term effects of stress on these implants.