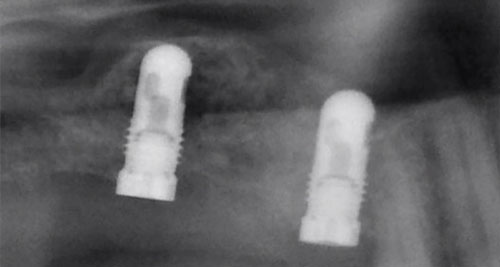
Bone grafting in the jaw
The aim of dental implants is to replace lost teeth. Similarly to the natural teeth they replace, the implants are anchored into the jawbone and fuse with the jawbone as part of natural biological processes. This was something discovered as early as in Egyptian times, or by the Etruscans, and by other highly-developed civilizations. The success rates were not, however, as high as they might have liked. In the 1960s, the Swedish physician I. Branemark stumbled upon a discovery: bone tissue grows and fuses with titanium surfaces very reliably. With this discovery, dental implants were born. In the years following this discovery, and over development to modern times, a ground-breaking new treatment area evolved for human medicine: orthopaedic and dental implantology.
As implants grow and fuse with the jawbone, the implantologist requires sufficient bone to work with in order to anchor the implant into place. It is unfortunately in just those places where implants are needed that no bone is left due to a process of bone deterioration. For many years, no implantation was possible in this scenario. Through years of intensive research, an effective surgical technique was developed for bone grafting (a way of ‘building bone back up’), which can make enough bone available at a desired location in nearly all patient circumstances.
Pathological alterations, e.g. predominating bone destruction (bone loss) is sometimes seen as osteoporosis, or in the cases of inflammation, periodontal disease, for example. Examples of excessive bone growth also exist, such as bone tumours.
In the mouth we see an example of when bone is rapidly lost: in cases of tooth loss. When teeth are really used and put under stress, bone is built up around the teeth and in the jawbone for stabilisation. This bone metabolism is particularly high in the inside of the bone: in the bone marrow, which due to its spongy structure is sometimes called spongiosa (or cancellous bone). The exterior outer hull of the bone, on the other hand, is very hard and exhibits reduced levels of metabolism: this is called the cortical bone. In the upper jaw there is a significantly greater proportion of cancellous bone; in the lower jaw, in contrast, there is more cortical bone. Specialists once thought that implants would hold better in the lower jaw due to increased hardness of the bone, but things aren’t, of course, that simple.
How do bones even grow?
In their growth phase, and also in the case of any breaks, bone cells (osteoblasts) are formed in the periosteum (outermost layer of bone), which produce hard bone substance in the surrounding area. Surprisingly, a parallel process of bone destruction also occurs alongside this bone formation process, carried out by another cell type, the osteoclast. The resulting bone is therefore alive: in a constant process of destruction and rebuilding. This process of cell control allows the body to very effectively adapt the quantity and density of bone in response to demands and stresses put on any region at a given time.

When do patients need bone grafting?
When teeth are lost, bone metabolism leads to immediate deterioration of the surrounding ‘woven’ bone (bone atrophy, or bone loss) as this bone is no longer needed. If a tooth, however, is to be replaced by an implant, patients must act fast in order for sufficient bone to still be available for implantation (within around 6 weeks). Once a few months pass since the tooth loss, a bone grafting treatment may be required, depending on each individual patient’s situation, in order to replace the lost bone for anchoring of the implants into the jaw bone. In order to make this type of assessment, implantologists need to carry out a thorough visual examination as well as carry out X-ray imaging. It is particularly common for bone grafting to be required in areas of the lower jaw and the side regions of the upper jaw (in the region of the maxillary sinuses).
Bone loss as a result of periodontal disease, however, more often than not means bone mass is lost in all areas. For each affected region and each extent and shape of remaining available bone, there is a special surgical technique. This is compounded by different surgeons’ preferences for different techniques and different types of bone replacement material. For non-experts, then, this field is not really something that can be fully understood, making it all the more important for patients to have an extensive consultation before having dental implants, even drawing on second opinions if required. Our dental implantologist are always delighted to see patients to give a full, extensive consultation and advise on treatment options. So you can get an idea of how the bone grafting procedure is carried out, below we have set out some of the techniques used:
“Our patients can benefit from the many years of experience in implantology, with our dentists working in the field for over 30 years. Using bone replacement materials, we are able to find solutions even in cases of patients having very little bone material left, and as a result, we can offer our patients long-term treatment solutions with implants and fixed dentures. As a rule of thumb, the bone grafting procedure requires a healing time of around 6 months.”
Dr. Michael Hager, Dentist at the Dr. Hager Dental Practice

Sinus-lift procedure using the method developed by H. Tatum, 1986
The most widely known version of the bone grafting procedure. Using strict scientific terminology, the procedure is referred to as sinus floor elevation, as the sinus floor must be raised up (i.e. elevated) due to the sinus floor now lying too low down following tooth loss. During the sinus-lift surgery, a so-called window is opened up in the side wall of the maxillary sinus using drills. The membrane covering the inside of the sinus can then be accessed (the “Schneiderian membrane”), and raised. This creates a space beneath the bony floor of the sinus and the raised membrane, into which an artificial bone replacement material is added. The desired implant can then be inserted during a second appointment (two-stage procedure), holding firmly in place. After a bone growth period of several months has passed, a large area of bone tissue will have grown into the treatment area, with natural, living bone cells and fine bone trabeculae (bone microstructures), making the structure robust and able to provide solid support for the implant.
Every implantologist has developed their own tweaks to the sinus lift procedure: we, for example, employ a minimally-invasive approach when creating the window into the sinus in order to leave as much bone as possible in the area available for subsequent growth. We also tend to insert the implants as part of the same sinus-lift procedure (unified, one-appointment procedure). We have made a decision against use of growth factors, in order to prevent uncontrolled cell division.
For the bone material added, we use exclusively synthetic bone replacement material, artificial bone, ruling out the possibility of any contamination by germs that might occur when using animal bone (e.g. cattle bone, Bio-Oss). Similarly, we do not use approaches that involve taking bone from the iliac crest (patient’s own pelvis area), as this causes pain for patients when walking over a prolonged period of time. The sinus-lift procedure ensures a high level of stability for implants made of titanium and ceramic.
Interner Sinuslift nach Summers 1994
This involves a modification of the sinus-lift procedure outlined above. In this procedure, a hole is drilled up into the maxillary sinus floor from below, with such precision as to reach the sinus floor but not break the interior membrane. The implant is then inserted directly into this hole. The internal sinus lift procedure is only safe where bone loss in the sinus is minimal. A modified version of the procedure involves adding bone material (including osteoblasts) from another location into the drilled hole before inserting the implant. This provides material for faster bone growth in this area, providing the solid bone basis required.
Another technique is the “sandwich graft”. This involves adding synthetic bone replacement material directly onto the site where bone has been lost. This material should only be in contact with the available bone lying beneath, from which bone cells can migrate into the material. All other tissues must be kept separated from the synthetic membrane inserted, as otherwise the faster connective tissue cells would penetrate into the bone replacement material. This would lead to no new bone growing. Here too, there are countless variations and methods available (bone splitting, bone spreading, …): even when merely discussing the materials used, experts at congresses quickly enter into hot debate.
As you can see, treatment approaches always depend on the biological growth effects of the natural bone, which the surgeon needs to take advantage of. As such, it is always the body itself which makes the desired healing process possible: the surgeon only optimizes the conditions for the body to carry out its work. In this respect, dentists must take the different capabilities for growth and immune defence strengths of individual patients into account. If need be, however, we can employ additional techniques and treatments in order to make the procedure a success. The duration of treatment extends over a period of several months where bone augmentation (grafting) is required, as we have to wait for the bone to grow.
We also welcome our patients to request a second opinion from another implantologist, and are more than happy to send our patients any X-ray imaging taken by email. In a similar fashion, patients often come to us for a second opinion, which we will always be happy to pass on to our colleagues with the highest levels of professionalism and providing our best assessments, without the need for accusations or reproaches.